Aboriginal and Torres Strait Islander women, the First Peoples of Australia, have been disproportionately affected by cervical cancer for decades, driven by long-standing systemic inequity, structural racism, and the absence of culturally safe, accessible cervical screening. It has previously been estimated that, nationally, Australia’s cervical cancer rates could fall below the WHO threshold for elimination by 2035, but it is not known when this could be achieved among Aboriginal and Torres Strait Islander women.
Considering the higher starting point for cervical cancer incidence rates among Aboriginal and Torres Strait Islander women than the general population, it is likely that specific action is needed to accelerate reductions and align with the national target of achieving elimination by 2035.
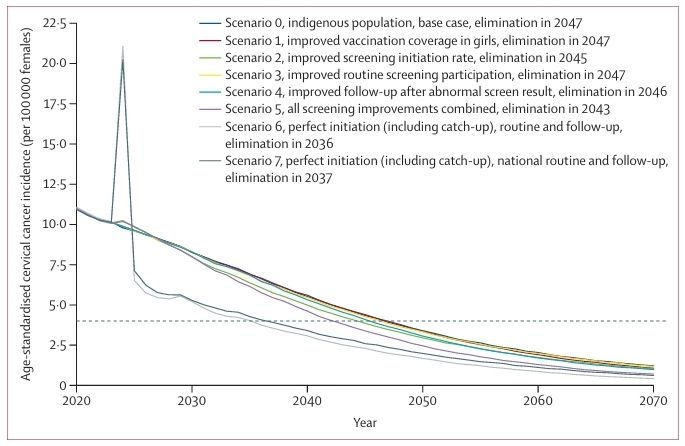
Our analysis predicted that, without change, cervical cancer elimination will be 21 years later for Aboriginal and Torres Strait Islander women than for the national population of Australia overall (2047 vs 2026, respectively), and 12 years later than Australia’s target of achieving equitable elimination by 2035. We found that systematic improvements to make screening more accessible and support timely follow-up that removed the difference in screening participation and follow-up rates could bring elimination forward to 2043, reducing the delay by 4 years. Increasing vaccination coverage to 90% seems unlikely to substantially expedite elimination timing, due to herd effects and one-dose vaccination coverage already being relatively high among Aboriginal and Torres Strait Islander females. However, the importance of high vaccine uptake in long-term cancer reductions should be noted. Since the current analysis was undertaken, more recent vaccine uptake data have been published, showing a decline overall but a more pronounced decline in Aboriginal and Torres Strait Islander than non-Indigenous adolescents.3
Our benchmarking analysis that considered scale-up to 100% screening, suggests that elimination could be accelerated by up to 11 years, within 1 year of the national 2035 goal; the key factor is to ensure every eligible Aboriginal and Torres Strait Islander woman is screened at least once. First, these findings suggest that matching the existing national rates should be a minimum, not a target. Second, they suggest that a major investment, now, in realising near-universal screening coverage in Aboriginal and Torres Strait Islander women would result in profound health outcomes within the next decade, achieve elimination as early as 2036, and could be expected to save lives, although quantifying these is beyond the scope of our analysis. Such a campaign would need to reach approximately 45 900 women in the near term. This could be achieved through an Aboriginal and Torres Strait Islander-led approach that prioritises culturally safe and impactful methods, such as selfcollection or point-of-care testing delivered via community co-designed pathways.19 Leadership from Aboriginal Community Controlled Health Organisations, supported by Aboriginal and Torres Strait Islander health workers and practitioners, will be essential to ensure the campaign is trusted, accessible, and responsive to community needs.5,20 New ways of addressing what has been a known inadequacy of the National Cervical Screening Program are required.
Under current vaccination and screening rates in Australia, the achievement of cervical cancer elimination among Aboriginal and Torres Strait Islander women was projected to occur in 2047 (figure 1, table 2). At the national level, elimination was projected to be achieved 21 years earlier, in 2026.
HPV vaccination and screening will in the long term decrease cervical cancer rates in Aboriginal and Torres Strait Islander women sufficiently to achieve cervical cancer elimination; however, without change, this is predicted to occur 21 years later than for other Australians. To achieve Australia‘s goal of equitable elimination as nearly as possible to the target timeframe of 2035, urgent action is imperative to ensure as many Aboriginal and Torres Strait Islander women as possible are supported to access screening and follow-up, and, in particular, a comprehensive effort to catch up those who have not screened previously.

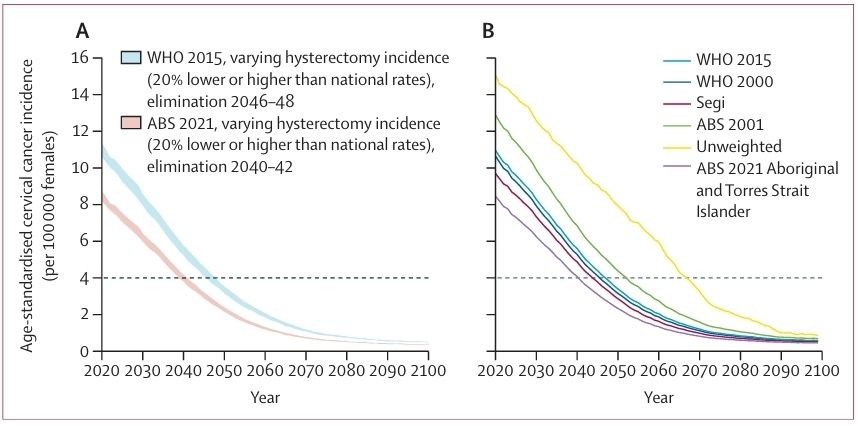
Sources;
Lancet Public Health 2026; 11: e197–201
Vol 11 March 2026